







| Sub Menu |
| History of the surgical treatment of breast cancer |
|
In addition to removing the tumor lymph nodes are still removed during a partial mastectomy not only to clear out any cancer cells that may have traveled to the nodes but more importantly to confirm whether or not there has been a spread of cancer. Positive nodes are an indication that the patient would need additional treatment such as chemo therapy because; positive nodes are a predictor of probable systemic spread of cancer. However removing lymph nodes from the axilla can have many draw backs including pain, numbness and swelling and since Women have greatly benefited from the sentinel lymph node biopsy an advancement first discovered in the 1980s when investigators in the field of melanoma (skin cancer) found that the injection of a certain blue dye into the cancer site would within moments travel under the skin through tiny invisible lymph channels to the nearest lymph nodes causing the first node to be stained blue. Identifying this node enabled us to remove fewer nodes and still be able to confidently confirm the cancers spread. The extension of sentinel lymph node biopsy to the treatment of breast cancer began at the John Wayne Cancer Institute in Santa Monica, California, in 1991. Unfortunately the blue dye method was only proven detectable in 60 % of cases. Other investigators used a radioactive substance injected around the cancer this in conjunction with a gamma ray hand held probe in the operating room was successful in locating the SLN 80% of the time. It was shortly after that we realized that utilizing the two methods together would allow us to successfully identify the SLN 97% of the time and is still the method being used today. |

Developed By
Scorpion Systems Web Design
Scorpion Systems Web Design

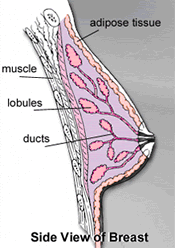 This is generally done using 7 weeks of external radiation (an external beam directed at the whole breast) but, can now also be achieved in a shorter period of time with less chance of radiating health tissue by utilizing the MammoSite® RTS (radiation therapy system) in which radiation is delivered in side the lumpectomy cavity (the space left after the tumor is removed).
This is generally done using 7 weeks of external radiation (an external beam directed at the whole breast) but, can now also be achieved in a shorter period of time with less chance of radiating health tissue by utilizing the MammoSite® RTS (radiation therapy system) in which radiation is delivered in side the lumpectomy cavity (the space left after the tumor is removed). we now know that removing all the nodes is not the answer because, it is not lymph node metastases that women die from but the spread to other vital organs.
we now know that removing all the nodes is not the answer because, it is not lymph node metastases that women die from but the spread to other vital organs.